Having a good sense of medical ethics is one of the most important parts of being a good doctor, but it is not emphasized as often as it should be. Proper medical ethics help support a proper doctor-patient relationship in which there is mutual trust and respect. However, many people have different views and values when it comes to what is ethical and what is not, making medical ethics quite complicated. In this post, we will explore the basic tenets of medical ethics and cases regarding them.

Medical Ethics Balance
The key principles of medical ethics are autonomy, beneficence, non-maleficence, and justice. While they may seem extraordinarily simple at first sight, we must unpack them to reveal their complexities. Autonomy refers to patients having full choice over their medical decisions. This entails telling the patient all of the medical details, not lying or leaving anything out no matter how bad it may be, so the patient can make an informed decision. For example, the doctor must tell their patients what is wrong with them, what their treatment options are, and what the associated risks are among other things. Doctors cannot force what they think is best for the patient upon the patient; although, they can offer their professional opinion if asked. This makes sense because patients should have control over their health and be able to do what they want to. Where this gets complicated is when dealing with people who may not be able to make decisions for themselves like children or the mentally ill. Then, you must turn to family, but what if family members disagree among themselves? Moreover, what if this child or the mentally ill patient chooses a treatment option or lack thereof that opposes the choice made by the family? Do you respect that or not? These questions have extremely difficult answers that can only be addressed on a case-by-case basis. The next major pillar of medical ethics is beneficence, which is to do things that benefit the patient. Doctors must always keep the patient’s welfare in the back of their minds. This also can be applied to a doctor’s obligation to medically help people even outside of the hospital. Whether this be through supporting public health initiatives or providing help in the event of a medical emergency on an airplane. However, this can easily get iffy. As Dr. Christopher Johnson explains, doctors sometimes do things that carry negligible benefit if any benefit at all for their patients like “a treatment or a test [that] is unlikely to help.” The next principle of medical ethics, nonmaleficence, is often closely related to beneficence. Nonmaleficence means to do no harm to the patient because a doctor’s job is to make the patient feel better, not worse. Part of this is that doctors should not offer false hope nor give treatments that are scientifically ineffective. For example, should you give chemotherapy, which is excruciatingly painful, to a patient with Stage 4 Cancer even if they have a poor prognosis whether they receive it or not? Proper acknowledgment of nonmaleficence means the doctors weigh the benefits and risks of the treatment, making decisions based on that. Justice is the last major part of medical ethics. In short, doctors must treat all patients equally regardless of their age, gender, socioeconomic status, religion, and sexuality among other things. This one is probably one of the simplest to understand, but it is also one of the hardest to implement. Doctors have inbuilt unconscious bias, which leads them to discriminate between patients sometimes unknowingly. For example, doctors are significantly more likely to view patients with substance use disorder more unfavorably than patients with mental health issues despite their both being chronic illnesses that are often outside the patient’s control. While autonomy, beneficence, nonmaleficence, and justice all are great principles and uniquely important to medical ethics, the questions associated with them prove that medical ethics is extraordinarily complicated.

Pillars of Medical Ethics
Dr. David Elkins is a psychiatrist who works at UCSF who told me a little about medical ethics. First, he told me about an interesting ethical case that he was a part of. There a woman in her 40s who refused a C-section despite clear evidence that the baby was in danger because she wanted a natural birth and did not believe in Western medicine. Her husband also wanted a natural birth but agreed that the doctors should do a C-section because the baby was in danger; however, she would not relent despite the doctors trying to explain to her that if she did not have a C-section, the baby was going to die. Should these doctors respect the patient’s autonomy or force her to have a C-section in the name of beneficence for the baby? Legally, a fetus is not a person until it comes out of the womb, so it was all up to the mother’s choice. Dr. Elkins was called in to do a mental health evaluation of the woman in order to make sure she was psychologically able to make this decision, and Dr. Elkins found that she was. Under increasing pressure, she finally agreed to the C-section. The baby needed antibiotics after it was delivered, but the mother said that she did not want the baby to be given antibiotics because it was Western medicine. Nevertheless, the doctors gave the baby antibiotics since the baby now was a separate living entity, and his life was at stake. Furthermore, Dr. Elkins brought up a thought experiment to imagine a world where drugs, alcohol, motorcycles, and guns are all banned. There are constant monitoring and privacy is limited, but the world becomes a much safer place at the cost of our freedom. Would you want to live in a world like that? Many rational people have drastically different answers to that question, making it one worth considering. Medical ethics can get confusing at times, and it is necessary to consider all sides of the equation before making a decision.
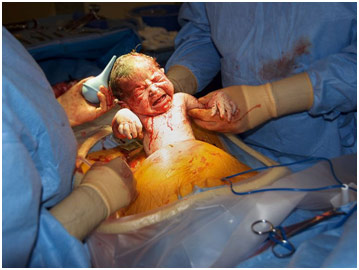
C-Section in Progress
Some of the most well known ethical codes in regards to medicine are the Hippocratic Oath and the Declaration of Geneva. A modern version of the Hippocratic Oath written in 1964 by Mr. Lasagna, the academic dean of Tufts Medical School, includes the principles of working together with other physicians, being able to admit when you need help, treating the patient and not the disease, seeking to always prevent disease rather than just treat it, and remembering the importance of patient confidentiality among other things. The Declaration of Geneva was adopted by the World Medical Association in 1948 and has been revised multiple times since then. Some of the principles it discusses are serving humanity, maintaining the honor of the profession, not discriminating against the patient on any basis, and respecting human life among other things. These codes reinforce the pillars of medical ethics that all doctors must abide by. With great power comes great responsibility; doctors have the power to save a patient’s life, but they also have the responsibility of doing right by this patient.
References
Johnson, Christopher. “The Basic Concepts of Medical Ethics Are Important for Everybody to Know.” ChristopherJohnsonMD, 13 Feb. 2014, chrisjohnsonmd.com/2014/02/13/the-basic-concepts-of-medical-ethics-are-important-for-everybody-to-know/. Accessed 10 Sept. 2017.
Medical Ethics. 12 Mar. 2017. Doctor to Be, doctortobe.co.uk/2664-2/. Accessed 10 Sept. 2017.
Six Values in Medical Ethics, Illustrated by Klimes Institute. Nursing Continuing Education, cecourses.org/ethics/care-ethics/palliative-ethics/. Accessed 10 Sept. 2017.
Statistical Analysis of Socioeconomic Factors Correlating to Caesarean Section Rates. Pinterest, pinterest.com/explore/baby-delivery-operation/. Accessed 10 Sept. 2017.
Three Person IVF: Law vs Ethics. 21 June 2016. Legal Seagull, legalseagull.org/tag/medical-ethics/. Accessed 10 Sept. 2017.
Tyson, Peter. “The Hippocratic Oath Today.” KQED, 27 Mar. 2001, pbs.org/wgbh/nova/body/hippocratic-oath-today.html. Accessed 10 Sept. 2017.
“WMA Declaration of Geneva.” World Medical Association, wma.net/policies-post/wma-declaration-of-geneva/. Accessed 10 Sept. 2017.