A few months back, I took a Stanford CME Course on a cardiovascular disorder called atrial fibrillation (AF). AF is one of the most common arrhythmias, which is an abnormal heartbeat, with more than 30 million cases of atrial fibrillation around the world. Diagnosing the disease early on is really important since leaving it untreated leads to a higher risk of a stroke since the patient has a higher probability of having blood clots as blood gathers in the heart. According to the American Heart Association, “untreated atrial fibrillation doubles the risk of heart-related deaths and is associated with a 5-fold increased risk for stroke,” which makes early treatment paramount. In a time where 610,000 people die annually of heart disease only in the US, knowledge about AF is what can save people’s lives and help find symptoms that may have otherwise been missed.
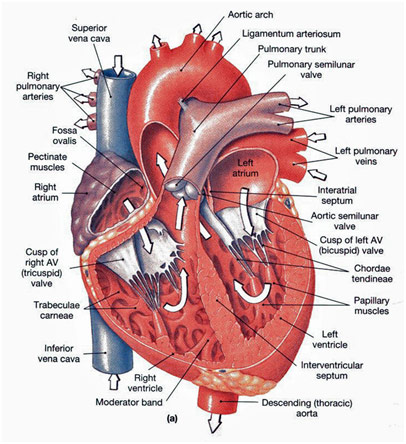
Anatomy of the Heart
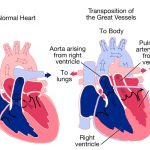
Atrial fibrillation specifically occurs because the upper chambers of the heart (atria) beat irregularly (fibrillate) due to abnormal electrical impulses to the heart. Specifically, these electrical impulses can be chaotic and start haphazardly from various places instead of only starting when needed from the sinoatrial (SA) node. Additionally, the atrioventricular (AV) node, which usually “serves as a ‘gatekeeper’ for all of the electrical pulses going through the atria (top sections) to the ventricles (bottom sections),” is unable to fulfill its job and limit the number of electrical impulses, according to the American Heart Association. Thus, instead of working smoothly, the heart is chaotic and is unable to pump blood throughout the body effectively. Multiple factors can cause this, but common causes include heart disease, heart defects, and sick sinus syndrome (sinoatrial node malfunction) among others.
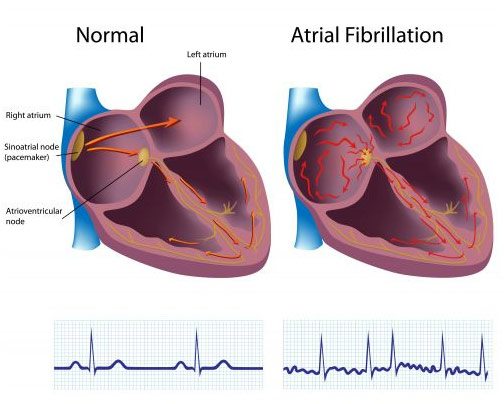
Anatomy and ECG of a Normal Heart and AF Heart
While symptoms often may help a diagnosis, an electrocardiogram is a gold standard for diagnosing AF. This is partly because 20-40% of patients do not experience any symptoms at all. For those that do experience symptoms, around half will have dyspnea, and other symptoms that occur in fewer than 30% of cases include chest pain, palpitations, dizziness, syncope, and fatigue. Since symptoms are not always conclusive and may mimic other conditions, a 12-lead ECG is a backbone of diagnosing AF. In the ECG, signs that the patient has AF include a “lack of P-waves, irregularly narrow QRS complexes, irregular cardiac cycles, and a wavy baseline,” according to Stanford. If these characteristics do appear in the ECG, the physician can start determining what kind of atrial fibrillation the patient has: paroxysmal AF, persistent AF, and permanent AF. Paroxysmal AF is when there are episodes of atrial fibrillation that come and go, usually never lasting more than 24 hours and stopping before one week goes by. Persistent AF is when these atrial fibrillation episodes go on for more than one week. Permanent AF is when treatment does not resolve the atrial fibrillation, and it is worth noting that paroxysmal AF and persistent AF can eventually become permanent AF if the episodes happen more and more often.
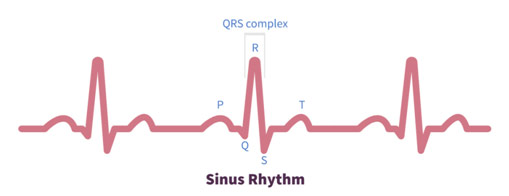
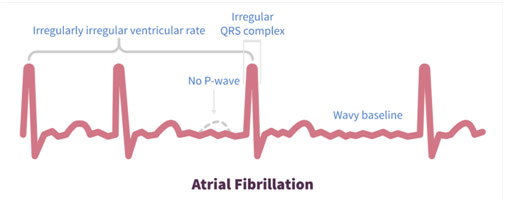
ECG for Normal Sinus Rhythm vs. Atrial Fibrillation
There are multiple different ways of treating AF, but most ways generally want to reduce the risk of a stroke, normalize ventricular rate, and normalize the heart’s rhythm. Reducing the risk of stroke is often done with anticoagulants; however, to see if the patient is a candidate for such therapy, a provider should use the CHA2DS2-Vasc scale to calculate if the benefits outweigh the risks. This basically means you go through a checklist: congestive heart failure (1 point), hypertension (1 point), age ≥ 75 years (2 points), diabetes mellitus (1 point), prior stroke/thromboembolism/TIA (2 points), vascular disease (1 point), age 65-74 years old (1 point), and sex is female (1 point). Current guidelines say that anticoagulant therapy should start for a patient with two points or higher. Drugs that are often used include warfarin, dabigatran, apixaban, edoxaban, and rivaroxaban. Warfarin works by blocking the formation of Vitamin K, which is an important part of creating clots. Dabigatran works by inhibiting thrombin, which is what causes clots in blood by making fibrin. Apixaban, edoxaban, and rivaroxaban all work by inhibiting the factor Xa, which makes thrombin from prothrombin zymogen. The second part is rate control to normalize ventricular rate to control the number of irregular heartbeats. The main drugs that should be used are beta-blockers like metoprolol, atenolol, carvedilol, and propranolol, and calcium-channel blockers like diltiazem and verapamil. Beta-blockers work by reducing the effect of epinephrine and norepinephrine, which reduces the number of electrical impulses that reach the AV node and slows down the patient’s heart rate. Calcium-channel blockers work by preventing calcium from entering the heart, which reduces the rate of electrical impulses that go across the AV node and slows down the patient’s heart as well. The third part is rhythm control to normalize the heart’s rhythm, which can be done with antiarrhythmic agents, cardioversion, or catheter ablation. Antiarrhythmic drugs include flecainide, propafenone, sotalol, amiodarone, dofetilide, and dronedarone. Flecainide and propafenone (class Ic antiarrhythmics) are both strong sodium channel blockers, which work by inhibiting the sodium entering into the heart, which slows the electrical impulses in the heart. Sotalol, amiodarone, dofetilide, and dronedarone (class III antiarrhythmics) are all potassium channel blockers, which work by inhibiting potassium entering the heart, which delays the repolarization of the ventricles (avoids early excitation of the heart muscle from next electrical impulse to avoid tachycardia). Along with pharmacotherapy, cardioversion is another viable option. Direct-current cardioversion works by using current by using an external defibrillator to shock a heart into a normal sinus rhythm. It is important to remember that cardioversion usually is only a temporary solution if the patient does not use antiarrhythmic drugs before and after the procedure. If both pharmacotherapy and cardioversion fail, catheter ablation is another option to treat atrial fibrillation. It works by destroying the parts of the heart that are causing problems. The doctor inserts a catheter through the femoral artery till it reaches the heart, and then the electrode on the catheter delivers energy that stops the tissue from triggering/transmitting electrical impulses. If it is radiofrequency ablation, the tissue will be destroyed with heat energy, and if it is cryoablation, the tissue with heat energy will be destroyed will cold temperatures. All in all, with quick diagnosis, treatment can be very effective in reducing the risk of serious complications from AF.
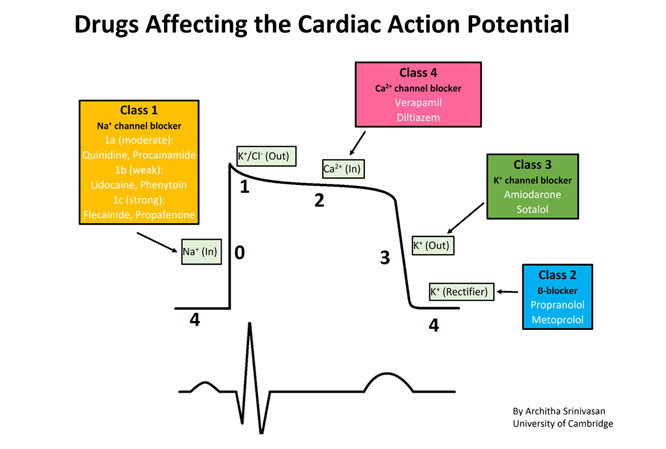
Pharmacotherapy for Rhythm Control of Atrial Fibrillation
Atrial Fibrillation has no cure, but with proper care, it is entirely possible to live a healthy life free of worry from serious complications. With more awareness, perhaps we will have fewer people who die or are severely crippled from a stroke, which was caused by AF. After all, proper management and treatment go a long way, which makes it really important to properly comply with a doctor’s instructions and prescriptions.
References
“Atrial Fibrillation.” Mayo Clinic, www.mayoclinic.org/diseases-conditions/atrial-fibrillation/symptoms-causes/syc-20350624. Accessed 2 Jan. 2018.
“Atrial Fibrillation.” NIH: National Heart, Lung, and Blood Institute, 14 Dec. 2015, www.nhlbi.nih.gov/health-topics/atrial-fibrillation. Accessed 2 Jan. 2018.
Auricles of the Heart. Anatomy, www.flspinalcord.us/auricles-of-the-heart/auricles-of-the-heart-heart-anatomy-chambers-valves-and-vessels-anatomy-physiology/#s. Accessed 2 Jan. 2018.
“CME: 021 Managing Atrial Fibrillation.” Stanford University, 20 Mar. 2017, cme.class.stanford.edu/courses/CME/021/2016/info. Accessed 2 Jan. 2018.
“Complications from Atrial Fibrillation.” Heart Rhythm Society, www.hrsonline.org/Patient-Resources/Heart-Diseases-Disorders/Atrial-Fibrillation-AFib/Complications-from-AFib. Accessed 2 Jan. 2018.
Drugs Affecting the Cardiac Action Potential. Wikipedia, en.wikipedia.org/wiki/Antiarrhythmic_agent. Accessed 2 Jan. 2018.
The Facts of AFib. Local SYR, www.localsyr.com/news/the-facts-of-afib-infographic/231005773. Accessed 2 Jan. 2018.
“Heart Disease Facts.” Center for Disease Control and Prevention, 28 Nov. 2017, www.cdc.gov/heartdisease/facts.htm. Accessed 2 Jan. 2018.
Klabunde, Richard. “Beta-Adrenoceptor Antagonists (Beta-Blockers).” Cardiovascular Pharmacology Concepts, cvpharmacology.com/cardioinhibitory/beta-blockers. Accessed 2 Jan. 2018.
—. “Calcium-Channel Blockers (CCBs).” Cardiovascular Pharmacology Concepts, www.cvpharmacology.com/vasodilator/CCB. Accessed 2 Jan. 2018.
Normal Vs. Atrial Fibrillation. Mid-Atlantic Cardiothoracic Surgeons, www.macts.com/heart-anatomy-and-rhythm.html. Accessed 2 Jan. 2018.
Pietrangelo, Ann. “Atrial Fibrillation by the Numbers: Facts, Statistics, and You.” Edited by Kenneth Hirsch. Healthline, 24 Dec. 2014, www.healthline.com/health/living-with-atrial-fibrillation/facts-statistics-infographic. Accessed 2 Jan. 2018.
“Why Atrial Fibrillation (AF or AFib) Matters.” American Heart Association, 22 Aug. 2017, www.heart.org/HEARTORG/Conditions/Arrhythmia/AboutArrhythmia/Why-Atrial-Fibrillation-AF-or-AFib-Matters_UCM_423776_Article.jsp#.WkVtOFQ-fys. Accessed 2 Jan. 2018.