Sleep disorders affect anywhere from 50-70 million Americans each year, costing nearly sixteen billion dollars. The most common one is insomnia; however, ones like obstructive sleep apnea, restless leg syndrome, narcolepsy, and REM behavior disorder are few others that also are quite serious. To understand how these disorders affect us, it is important to understand what sleep consists of. NREM (non-rapid eye movement) sleep and REM (rapid eye movement) sleep are the two sleep cycles. NREM, which is split up into four stages, mainly consists of the slowing down of brain waves while muscles begin to relax. In addition, heart rate, blood pressure, and body temperature are all depressed as these stages go on, sinking to their deepest levels in stage 3 and 4 NREM sleep. One’s body cycles between NREM and REM sleep where REM periods become longer and longer as the morning hours creep by. In REM sleep, a person’s brain activity is characterized by its similarity to the same person’s brain activity when they are awake. There is also atonia during this time, which is just the paralysis of the muscles aside from those needed for vital functions. After multiple of these cycles, one wakes up and it is morning. Sleep disorders can profoundly disrupt this carefully tuned process, which necessitates being aware of them. This post discusses some of the most common sleep disorders and is the second part of a two-part series on sleep medicine.
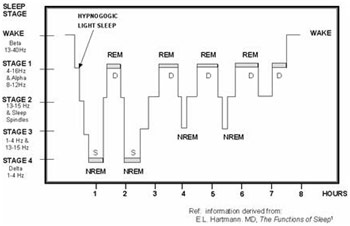
Sleep Stages and Cycles
REM behavior disorder (RBD) occurs when the muscles do not paralyze during REM sleep like they are supposed to. Thus, people with this disorder act out their dreams by talking, walking, punching, etc without even consciously knowing that they are doing it. The exact cause of RBD in most patients is unknown but is thought to be due to the degradation of nerve pathways that control this paralysis of muscles. Indeed, it is very common in elderly people and people who have neurodegenerative disorders, especially Parkinson’s disease. While Parkinson’s is a risk factor, it is also a disease that often succeeds RBD. Nearly forty percent of people with RBD developed Parkinson’s in 12 to 13 years in a study. To diagnose the condition, the doctor can do polysomnography where the heart rate is monitored with an electrocardiogram (ECG), the brain activity with an electroencephalography (EEG), the eye movement with electrooculogram (EOG), and the muscle movements with an electromyogram (EMG) among others like lung activity and blood oxygen levels. By ruling out other sleep disorders, observing that there is no atonia, and noticing vocalization/movement, one can be diagnosed with RBD and began to be treated with clonazepam, which is a benzodiazepine and works by reducing muscle activity. Taking a low dose a little before bedtime helps in nine out of ten cases of RBD. With proper treatment, RBD is an entirely manageable disease.
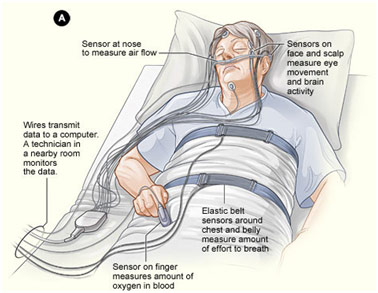
Polysomnography Test Setup
Narcolepsy occurs when the brain is unable to control sleep and wakefulness. People with this disorder may suddenly enter REM sleep without much warning. It is often accompanied by cataplexy where there is a sudden loss of muscle tone, which can be triggered by a variety of emotional experiences like laughter or fear. People who experience cataplexy may not be able to move at all, similar to the experience of having atonia in REM sleep, except for the fact that a person is actually awake during cataplexy. People with narcolepsy may also experience hypnagogic hallucination as they enter a dreaming state while partially awake or hypnopompic hallucination as they leave a dreaming state while partially awake. There is no exact cause, but for most people, the problem is autoimmune in nature as there is an attack of nerve cells in the lateral hypothalamus that contains the neurotransmitter orexin, or hypocretin, which regulates wakefulness. Thus, these people have low levels of hypocretin and find it hard to stay awake as they are almost always drowsy. There also may be an association of narcolepsy between infections like swine flu and strep throat; however, that is still being researched at the moment. To diagnose the condition, doctors often do polysomnography with the same tests being done as for REM behavior disorder and multiple sleep latency tests where one is “asked to nap for 20 minutes every 2 hours throughout the day” according to the US Department of Health & Human Services. By seeing if one falls asleep quickly and enter REM sleep quickly, these tests can help determine if the patient has narcolepsy. Stimulants like methylphenidate (Ritalin) or Provigil (modafinil) are used to reduce daytime sleepiness. Tricyclic antidepressants like Anafranil (clomipramine) or selective serotonin reuptake inhibitors like fluoxetine (Prozac) are used to treat cataplexy. As one can see, these drugs treat the symptoms, not the cause. Narcolepsy is a lifelong condition, but by making some lifestyle adjustments and taking some medication, living with the condition can become easier.
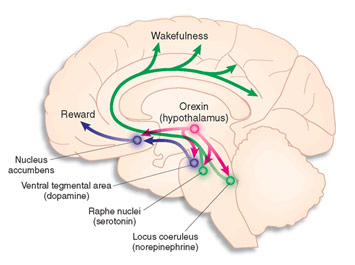
Orexin Pathways in the Brain
Restless Leg Syndrome (RLS) is a disorder characterized by an uncomfortable “pins and needles” feeling in one’s legs and an uncontrollable need to move them. The symptoms usually present themselves or are worst at night as they occur in response to a desire to sleep. According to the National Institute of Neurological Disorders and Stroke, people with the disorder have difficulty sleeping, and many are “unable to concentrate, have impaired memory, or fail to accomplish daily tasks,” making treating this disorder extremely important to better these people’s quality of life. The exact cause of this disorder is unknown, but it is thought to be linked to genetics: almost one in two people with RLS also have a family member with the condition. Some evidence also indicates that it is related to a problem with the basal ganglia in the brain, which uses dopamine, as a lack of the brain chemical causes uncontrollable movements. There are five criteria used to diagnose the condition: there is an uncontrollable urge to move one’s leg due to discomfort, the urge is aggravated when one is at rest, the urge is also worsened at night, the urge is somewhat relieved by moving the legs, and they are not caused by any other medical condition, which is usually done with laboratory tests and sometimes polysomnography. Lifestyle changes are always recommended to treat RLS: doctors may tell the patients to change their sleep pattern, start a regular exercise regimen, and avoid drugs like nicotine, alcohol, or caffeine. In terms of pharmacotherapy, there is no one drug that cures RLS, but there are ones that help treat it. One commonly prescribed drug class is anticonvulsants like gabapentin (Neurontin) and gabapentin enacarbil (horizon) that prevent abnormal electrical activity in the brain, working to help reduce nerve pain. Another common drug class is dopaminergic agents like ropinirole (Requip) or carbidopa/levodopa (Sinemet), which increase dopamine levels in the brain and actually reduce symptoms like stiffness and tremors. Benzodiazepines and opioids are also sometimes used to help give a more restful sleep and treat severe symptoms, but they tend to be only reserved for more extreme cases as they can both be abused due to their addictive qualities. Once again, RLS is usually a lifelong condition but a manageable one at that if diagnosed and treated correctly.

Restless Legs Syndrome Infographic
Obstructive Sleep Apnea (OSA) is a sleep disorder where breathing becomes shallow or suddenly stops while asleep. One of the biggest symptoms and perhaps the biggest indicators that one has OSA is loud snoring as the snoring occurs when flowing air is obstructed. Due to these periods of shallow or stopped breathing, there can be a lack of oxygen flowing to vital organs, which can lead to complications like cardiac arrest, hypertension, and stroke among others. Additionally, patients with OSA can have fatigue and feel sleepy during the daytime as they cannot reach deeper stages of their sleep cycle. This is because their brains wake the patient up when they are not breathing properly in order to temporarily increase blood oxygen levels; this can happen hundreds of times a night. OSA is caused usually either by the relaxation of muscles in the back of the throat that are meant to keep the throat open or physical obstructions like enlarged tonsils, tongue, or adenoids. Obesity can also cause or increase the risk of OSA since fat tissues can cause yet another physical obstruction. Once again, polysomnography is done with a special focus on airflow and blood oxygen levels since those results can help diagnose the condition by seeing how often the patient’s breathing was unnatural. Also once again, lifestyle changes are recommended: losing weight, quitting smoking/reducing alcohol intake, exercising, and sleeping on the side instead of on one’s back are all recommendations. Additionally, there are breathing devices that can help treat this condition like continuous positive airway pressure (CPAP), the most common and most successful therapy, which has constant pressured air enter the patient’s body to keep the airway open. Other therapies like having a mouthpiece, which works to keep the patient’s mouth open usually by moving the jaw forward, are popular. There are many surgical interventions as well. Uvulopalatopharyngoplasty (UPPP), the most common surgical procedure, is done to remove some tissue like the tonsils/adenoids, uvula, or soft palate from the patient’s throat. Maxillomandibular advancement can also be done where the maxilla (upper jaw) and mandible (lower jaw) are moved forward to allow for more space in the back of the throat, which reduces the chance of there being an obstruction. Additionally, devices can be surgically implanted to treat OSA. One type that is implanted in the upper chest works by stimulating the hypoglossal nerve to move the tongue if breathing is impaired. In the most extreme of cases, a tracheostomy may be done where a surgical opening directly in the windpipe is made so the patient can use the trach tube instead of the blocked air passage for breathing. Certainly, there are many diverse therapies for OSA, which allow for management to be entirely possible.
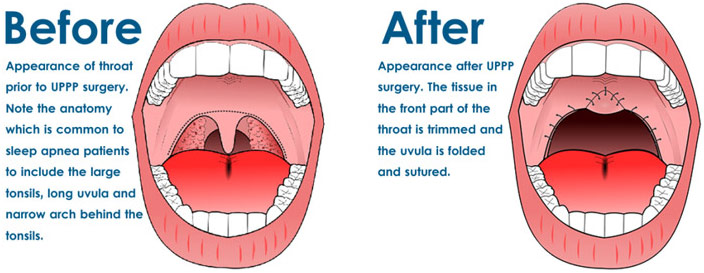
Before and After Pictures of Uvulopalatopharyngoplasty
Insomnia is a disorder characterized by difficulty while sleeping, whether it be falling asleep initially, staying asleep, or returning back to sleep. It is often associated with poor sleep quality, which can cause fatigue, anxiety, and difficulty with tasks like learning among other things. It is also worth noting that insomnia can be categorized into chronic insomnia and acute insomnia; however, we will focus on chronic insomnia mostly for this post. Chronic insomnia can be caused by stress that keeps one awake and poor sleep habits that interfere with the body’s natural circadian rhythm (sleep cycle). Additionally, other disorders like anxiety disorder, Parkinson’s, and lower back pain can keep one up during the night. Sometimes, stimulants like caffeine and nicotine can keep one awake while depressants like alcohol can prevent one from being able to enter the more restful stage of NREM sleep. Diagnosing insomnia is again done through polysomnography along with a sleep diary to review sleeping habits and the Epworth Sleepiness Scale, which measures daytime sleepiness through a questionnaire. It can be used for other sleep disorders as well, but it is not the best test as it is quite subjective. Pharmacotherapy for insomnia is usually done with sedating benzodiazepines like triazolam (Halcion), sedating nonbenzodiazepines like zaleplon (sonata), melatonin receptor agonists like ramelteon (Rozerem) which is sedating due to the artificial melatonin’s effect on the sleep-wake cycle, and orexin receptor antagonists like suvorexant (belsomra) which block the formation of orexin that regulates wakefulness as mentioned before. Sometimes, these drugs are combined with cognitive-behavioral therapy (CBT-1) which combines changing negative thoughts/emotions about one’s own ability to sleep with developing good sleep habits to combat negative sleep behavior. Even though this sleep disorder is the most common one of them all, it too can be treated.
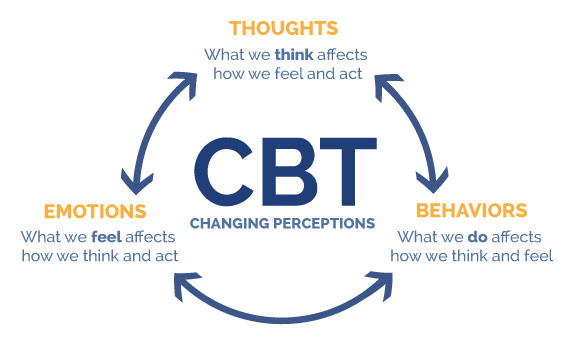
Basis of Cognitive Behavioral Therapy
Sleep disorders can seriously affect one’s quality of life, which is why proper treatment is paramount. Most drugs treat the symptoms, not the underlying problem, which is why further research is needed to find a cure that solves these disorders once and for all.
REFERENCES
https://www.sleepassociation.org/sleep/sleep-statistics/
https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Understanding-Sleep
https://www.medicalnewstoday.com/articles/247730.php
https://www.webmd.com/sleep-disorders/diagnosing-rem-sleep-behavior-disorder
https://www.mayoclinic.org/diseases-conditions/narcolepsy/symptoms-causes/syc-20375497
https://www.nhlbi.nih.gov/health-topics/narcolepsy
https://www.webmd.com/sleep-disorders/narcolepsy-treatment
https://www.webmd.com/brain/restless-legs-syndrome/restless-legs-syndrome-rls#1
https://www.webmd.com/sleep-disorders/guide/understanding-obstructive-sleep-apnea-syndrome#2-4
https://www.nhlbi.nih.gov/health-topics/sleep-apnea
https://www.mayoclinic.org/diseases-conditions/insomnia/symptoms-causes/syc-20355167
https://www.webmd.com/sleep-disorders/diagnosing-insomnia
https://www.webmd.com/sleep-disorders/understanding-insomnia-treatment#1
https://www.mayoclinic.org/diseases-conditions/insomnia/diagnosis-treatment/drc-20355173










I’m really happy with the comfort of the mask and am encouraged that I’ll transition to using CPAP in a relatively short period of time.