Recently, I took a UPenn CME Course on a cardiovascular disease called hypertension or commonly known as high blood pressure. Blood pressure is defined by the systolic and/or diastolic pressure. Systolic pressure is the pressure when the left ventricle of the heart contracts and pushes oxygen-rich blood throughout the body while diastolic pressure is the pressure when the left ventricle fills with this oxygen-rich blood. Usually, hypertension is diagnosed with a systolic blood pressure of at least 130 mm Hg over a diastolic pressure of at least 80 mm Hg. This basically means that the pressure pushing on the left ventricle and other blood vessels is far too high. This is significant because higher blood pressure increases the chance of heart attack, stroke, kidney failure, and vision loss among others. In the BP Trialists study published in 2003, it was found that for every increase of 20 mm Hg of systolic pressure, the risk of dying from a stroke along with ischemic heart disease doubled (Lewington et al). One in three adults in the US are diagnosed with hypertension, and the risk of being diagnosed with it increases with age. Specifically, three-fourths of women and two-thirds of men over the age of 75 have hypertension, making detection and early management extremely important.
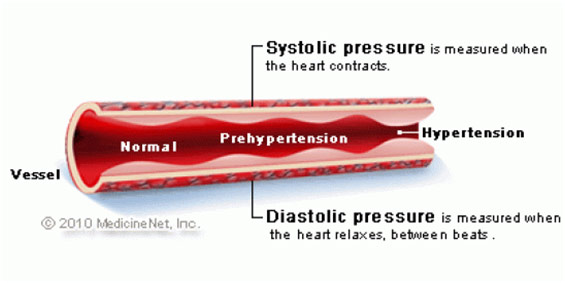
Blood Vessel Blockage as Hypertension Progresses
Hypertension is associated with blood vessels narrowing, forcing the heart to work harder to pump oxygenated blood throughout the body. While the exact cause for why this happens is unknown, many different factors can influence and cause hypertension. Often, this occurs in conjunction with the buildup of LDL cholesterol (the “bad cholesterol”), which forms plaque, in the arteries, making it even harder to pump blood through them. Other contributors include smoking because nicotine narrows arteries, obesity, and elevated salt intake because salt pulls water into the arteries increasing the volume that has to pass through them, and because salt enhances the body’s response to other influences that raise blood pressure. Hypertension is often labeled the “silent” killer because it generally causes no noticeable symptoms and can escalate to morbid diseases. For example, there can be an aneurysm, which is when a bulge forms in an artery and has the potential to rupture, which may cause life-threatening internal bleeding. Another complication is a stroke which is when there is an acute reduction in the delivery of oxygenated blood to the brain, sometimes due to a blood clot in the arteries leading up to the brain, causing a part of the brain to die. Moreover, heart failure is yet another complication that happens because the heart is overworked due to the higher pressure against which it beats, and like other muscles, it thickens to meet the body’s needs. Ultimately, it becomes strained because it can no longer adapt, leading the heart to fail. The last major complication that I will talk about is kidney failure, which is when there is damage to the renal arteries (the arteries leading to the kidneys) and the circulation within the kidney itself. Thus, the kidneys can potentially become inefficient in filtering waste, which builds up waste in the body, causing a patient to require dialysis or a kidney transplant down the road when this buildup becomes symptomatic. Moreover, as the kidneys fail, the body often “pushes” them to work harder by raising the blood pressure to force them to filter more blood. These are just a few of the main complications, and it’s important to remember that there are many more.
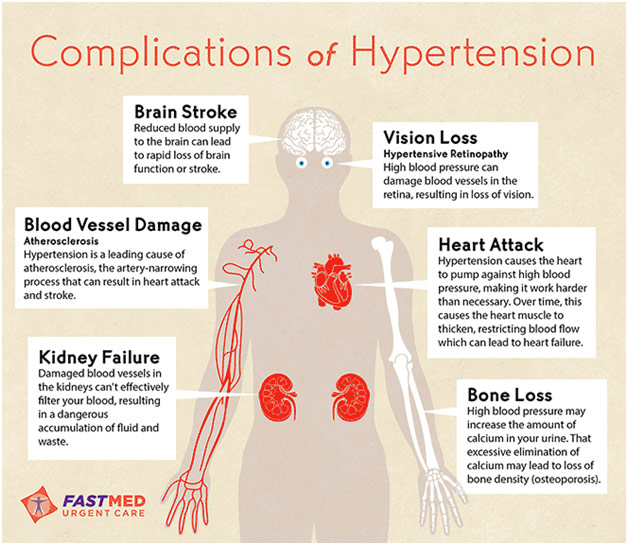
Complications of Hypertension
Thus, it becomes extremely important to constantly check for the blood pressure at every clinical visit to be able to detect hypertension early on. Many times, lifestyle changes can be very helpful. For example, exercising and losing weight can make a big difference in lowering blood pressure. Moreover, eating healthy (guidelines in the DASH diet) and reducing stress are other good changes to help high blood pressure. However, from a pharmacologic therapy standpoint, there are multiple different types of drugs a hypertensive patient can take to fix their blood pressure along with making the lifestyle changes talked about above. There are four main groups of drugs relevant to hypertension that I will discuss: thiazide diuretics, RAS system inhibitors, beta-blockers, and calcium channel blockers. Thiazide-type diuretics take out excess water and salt from your body (specifically by inhibiting sodium-chloride cotransporter in the kidneys) to decrease the pressure going through the blood vessels. RAS (renin-angiotensin-aldosterone) system inhibitors are all about the system where the body secretes the enzyme renin, which produces angiotensin (narrows blood vessels). Angiotensin increases the production of aldosterone (more absorption of salt and water in the blood), subsequently increasing blood pressure. There are two RAS subclasses: ACE-I (angiotensin-converting enzyme inhibitors) and ARA (angiotensin receptor antagonists). ACE-1s reduce the transformation of nonfunctioning angiotensin I into functioning angiotensin II. ARAs work by impairing the ability of angiotensin II to bind to receptors, effectively stopping it. Beta-Blockers work by making your heartbeat slower and less forcefully. Lastly, CCB (calcium channel blockers) work by reducing calcium into cells in the blood vessel muscle layer which gives blood vessels their “squeeze” or constriction, which in turn reduces blood pressure by relaxing the blood vessels directly.
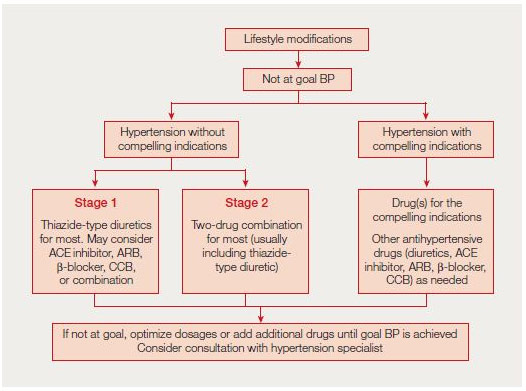
Treating Hypertension According to new ACC/AHA and older JNC-7 Guidelines
Often, multiple different drugs are needed along with lifestyle changes in order to get control of hypertension and to reduce it to a normal level. Thus, it is really important to follow the doctor’s prescription and advice to properly maintain hypertension in the long run. With proper care, it is entirely possible to lead a normal healthy lifestyle free of complications.
References
Cassata, Cathy. “High Blood Pressure Medications.” Edited by Sanjai Sinha. Everyday Health, 2017, everydayhealth.com/high-blood-pressure/guide/medications/. Accessed 13 Sept. 2017.
Complications of Hypertension. FastMed Urgent Care, fastmed.com/services/urgent-care-services/illnesses-and-injuries-treated/high-blood-pressure-hypertension/. Accessed 13 Sept. 2017.
“JNC 7: Algorithm for Hypertension Management.” Medicographia, medicographia.com/2012/07/combination-therapy-in-the-management-of-hypertension-which-one-for-which-patient/. Accessed 13 Sept. 2017.
Lewington, et al. “Age-specific Relevance of Usual Blood Pressure to Vascular Mortality: A Meta-analysis of Individual Data for One Million Adults in 61 Prospective Studies.” PubMed, 14 Dec. 2002, ncbi.nlm.nih.gov/pubmed/12493255/. Accessed 13 Sept. 2017.
Mayo Clinic Staff. “Choosing Blood Pressure Medications.” Mayo Clinic, 2017, mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/high-blood-pressure-medication/art-20046280. Accessed 13 Sept. 2017.
—. “High Blood Pressure Dangers: Hypertension’s Effects on Your Body.” Mayo Clinic, 23 Nov. 2016, mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/high-blood-pressure/art-20045868. Accessed 13 Sept. 2017.













Are you gonna to share more concerning this subject? I intuit you might be downplaying some of your more controversial reasoning, but I for one, love hearing them!