Virtual Reality (VR) is often in the headlines for being the future of gaming. Yet, this tool seems likely to play a substantial role in the future of medicine to help patients, medical students, and doctors alike. If you think about it, the ability to visualize a three-dimensional field in such detail that it feels like a true human experience has enormous potential to transform medicine. With the widespread adoption, patients could feel less pain, the medical learning experience could be raised to a whole new level, and operations could become safer. Thankfully, this technology is being implemented and changing lives as we speak.
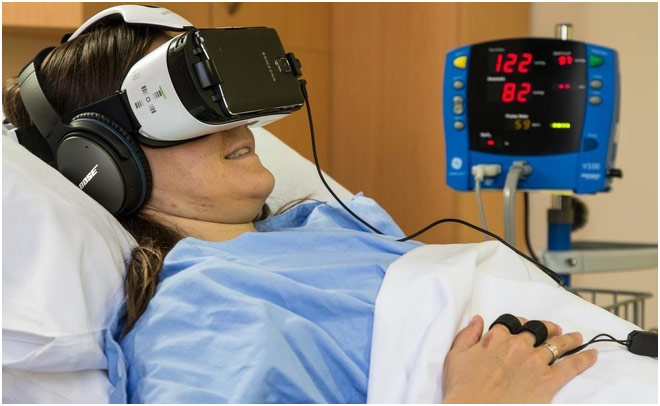
Patient Using VR in a Hospital
VR can help distract patients from their pain, effectively lessening the intensity in the moment and also in the long run as few studies have proved. The basis behind it is to work off mirror therapy, which has been proven to be successful in reducing pain in patients with amputations or lost limbs that cause phantom limb pain. Basically, mirror therapy is done by using a mirror to show a patient a reflection of their unaffected limb in a way where they are visually stimulated to believe that they are able to move the affected limb. This helps alleviate the pain normally “caused by the brain attempting to move the absent limb, sending out abnormal neural patterns which are experienced as shooting pain” since the brain can see the affected limb move and get over the pain. VR improves on this therapy since it is able to create a virtual limb that seems more realistic, which means the patient is more likely to feel less pain since the patient feels like they are making normal movements in real-time for the affected limb. However, VR is not limited to just helping patients who have lost a limb since it can also be extremely helpful for treating burn victims. For some burn patients, who experience an extraordinary amount of pain during wound care, opioids do not help alleviate the pain enough, and this is where VR comes in since it has been able to alleviate a lot of the pain through distraction. Using VR games like SnowWorld, which was made by the University of Washington, patients are drawn into the wintery wonderland, allowing them to escape paying attention to their pain, which means they, in turn, feel less acute pain; this is known as the gate theory of pain. VR has even been shown to help people with chronic pain like from diseases such as neuropathy, which is pain due to nerve damage. According to a study led by Dr. Jones, there was a 60% reduction in pain from before the VR session to during the VR session and a 33% reduction in pain from before the VR session to after the VR session. Thus, VR provides a more cost-effective and safer way to treat a patient’s pain, making it more viable as the future of pain management.

A Picture from the VR Game SnowWorld
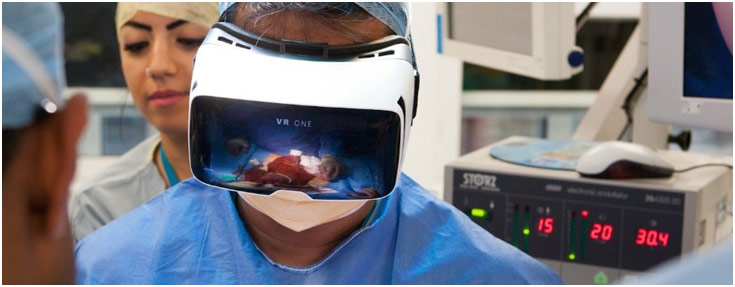
The way medical training is occurring is also changing from live-streaming operations with the VR headset to learning how to empathize with older patients by virtually walking in their shoes. In April 2016, Dr. Shafi Ahmed from London streamed his operation that could be seen by anyone in the world who had access to a phone or computer. He walked the viewers step-by-step through the operation to remove the cancerous tissue from a real patient’s colon as well as answered questions out loud while he operated from people who typed them while watching the procedure. The 360-degree experience is what made this extremely special as viewers can immerse themselves in the surgery with all of the sights and the sounds. Additionally, medical students and residents can refer back to videos like this and others to re-familiarize themselves with the operation before they have to go in to observe or assist the surgeon. However, VR plays an even more important educational role outside of simple observation since it is also supplementing anatomy lessons from the cadaver lab with ones from the virtual reality lab. In UCSF for example, medical students are able to take layer by layer of the human body apart virtually to a three-dimensional view of the anatomy and how the structures work. Additionally, virtual patients can be programmed in order to train the medical student how to work with their medical team, communicate effectively, and operate well in high-stress environments. Empathy is also an important skill for doctors, which is where We Are Alfred is coming in. The program created by Embodied Labs allows medical students with VR headsets to experience 7 minutes in the shoes of Alfred, who is almost 75-years-old and is severely impaired. The experience allows these students to commiserate with the ordeals that will be felt by their future patients. Indeed, work like this is making better doctors by improving their training.

We Are Alfred Simulation
VR is not only for patients and medical students though as doctors are now using it to make their surgeries safer by planning them in advance. Stanford has been one of the hospitals to take the lead with this since they often use VR to combine scans like CT or MRI, which normally use “3D perspectives on a 2D screen,” to create a virtual three-dimensional structure. Using technology like True 3D, the surgeon can view the anatomy in detail, anticipate potential difficulties, and test the feasibility of more minimally invasive surgeries. For example, the team that separated a pair of conjoined twins at Stanford used VR technology to examine complex steps in the operation and determine how best to go around it with a 3D virtual representation of the twins. VR helps surgeons plan the surgery and reduces the chance that they will be surprised while doing it since they know exactly where best to make the incisions and were best to avoid. This is especially true for smaller hospitals that receive a rare case, which none of the surgeons have operated on since they can go through all of the motions with VR. Thus, VR is allowing surgeons to improve mortality rates and make the patient experience much better.

Surgical Residents Observing the Anatomy in a Skull
Patients, medical students, and doctors alike should rejoice in the more widespread use of VR technology. For patients, they can have both chronic and acute pain reduced in a way that is engaging and immersive. For medical students, the quality of their education is only improving since they can observe surgeries in real life or examine a virtual human body, layer by layer. For doctors, they can plan out complex operations to ensure they are doing the best job they can when they operate on their patients. The future of medicine seems to be going in the right direction with the use of VR.
References
Baker, Mitzi. “How VR Is Revolutionizing the Way Future Doctors Are Learning about Our Bodies.” University of California San Francisco, 18 Sept. 2017, www.ucsf.edu/news/2017/09/408301/how-vr-revolutionizing-way-future-doctors-are-learning-about-our-bodies. Accessed 19 Dec. 2017.
Digitale, Erin. “Virtual Reality Imaging Technology Gives Surgeons a Better View into Patient Anatomy.” Stanford Children’s Hospital, www.stanfordchildrens.org/en/about/news/releases/2017/virtual-reality-imaging-technology-makes-surgery-safer. Accessed 19 Dec. 2017.
Echopixel. www.echopixeltech.com/true-3d-viewer/. Accessed 19 Dec. 2017.
“5 Ways Medical VR Is Changing Healthcare.” Medical Futurist, 1 Apr. 2016, medicalfuturist.com/5-ways-medical-vr-is-changing-healthcare/. Accessed 19 Dec. 2017.
Helm II, Standiford. “Mirror Therapy for Phantom Limb Pain.” Edited by Melissa Conrad Stöppler. Medicine Net, www.medicinenet.com/script/main/art.asp?articlekey=88097. Accessed 19 Dec. 2017.
Johansen, Mogens. Patient Using VR. WordPress, 2 Apr. 2016, socialvrblog.wordpress.com/2016/04/02/treating-psychological-factors-in-cancer-patients-using-virtual-reality-treatment-vrt/. Accessed 19 Dec. 2017.
Jones, T., et al. “The Impact of Virtual Reality on Chronic Pain.” Pub Med, 20 Dec. 2016, www.ncbi.nlm.nih.gov/pubmed/27997539. Accessed 19 Dec. 2017.
Magid, Larry. “Virtual Reality Can Help Alleviate Pain.” The Mercury News, 15 June 2017, www.mercurynews.com/2017/06/15/virtual-reality-can-help-alleviate-pain/. Accessed 19 Dec. 2017.
Sakuma, Paul. The Virtual Reality System Is Helping Train Residents, Assist Surgeons in Planning Upcoming Operations and Educate Patients. It Also Helps Surgeons in the Operating Room, Guiding Them in a Three-Dimensional Space. Stanford Medicine, 11 July 2017, med.stanford.edu/news/all-news/2017/07/virtual-reality-system-helps-surgeons-reassures-patients.html. Accessed 19 Dec. 2017.
A Virtual Reality Experience Transforms the User into a 74-Year-Old Named Alfred in Order to See His Perspective as a Medical Patient. UIC Today, 17 May 2016, today.uic.edu/east-meets-west-we-are-alfred. Accessed 19 Dec. 2017.
“Virtual Reality Pain Reduction.” Human Photonics Laboratory, www.vrpain.com/. Accessed 19 Dec. 2017.
“VR and Mobile Technology Is Changing the Way Medical Students Learn.” Vice, 12 Sept. 2016, www.vice.com/en_uk/article/5geq4q/vr-and-mobile-technology-is-changing-the-way-medical-students-learn-o2-newnormal. Accessed 19 Dec. 2017.