Like many other professions, medicine has been subject to some automation in recent times. Already machines can read EKGs and detect suspicious masses in mammograms among other things. Additionally, deep learning has transformed the limits of what automation has the potential to do. Being fed images along with their proper diagnoses, automated machines have the ability to teach themselves, and eventually, they can look for certain indicators to make proper diagnoses themselves (Mukherjee). This development is significant since, in general, machines are more specific and sensitive in making diagnoses than their human counterparts. For example, there was a study performed in Sweden where Dr. Hans Ohlin, the chief of coronary care at the University of Lund Hospital and a person who read thousands of EKGs annually, competed with a machine to see who could determine which patients had a heart attack and which patients did not (Gawande 37). In the end, the machine beat man by some 20%, diagnosing more heart attacks correctly (37). Machines are not just limited to making diagnoses as they may be able to treat patients and carry out surgeries on patients as well. While the full role that automation will play in the future is unclear, doctors may find machines to be an extremely powerful tool in their arsenal to improve healthcare and medicine. Missed diagnoses could become a thing of the past and surgeries could become significantly faster and less invasive as preventative medicine thrives; however, the ethical concerns must be weighed before automation is fully integrated into the medical field.
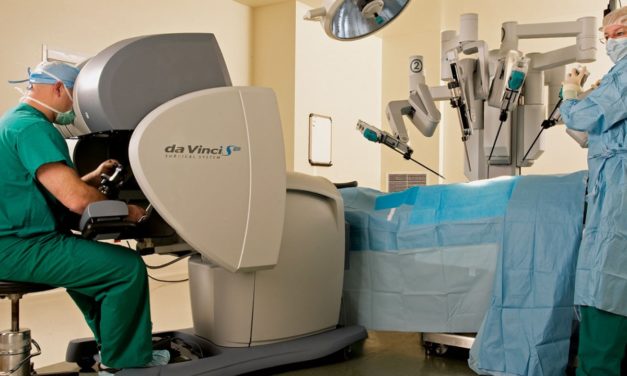
A da Vinci Surgical System in the Operating Room
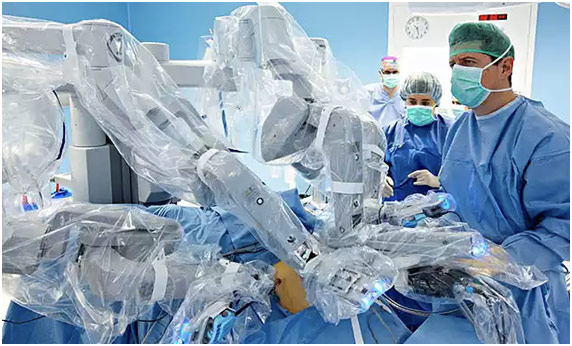
Intuitive Surgical’s da Vinci Surgical System and the Smart Tissue Autonomous Robot both represent different levels of automation in the medical field. The da Vinci Surgical System is used to perform many different minimally invasive surgeries; however, unlike the other example, it is entirely surgeon driven since it allows the surgeon to work from a console, maneuvering the four arms of the robot as it operates on the patient. With the view of the patient’s anatomy through the high definition 3D camera, the surgeon is able to make simple hand movements, which translate into extremely precise motions done on the patient in real-time (Robotic Surgery). The robot has enormous potential to make minimally invasive surgeries, which provide significantly better outcomes than more invasive types of surgeries since these often have a higher risk of infections and longer recovery periods, quicker and easier to perform (Robotic Surgery). Furthermore, the da Vinci Surgical System represents a non-problematic type of automation since it simply enhances the surgeon’s abilities rather than replaces the surgeon outright. Nevertheless, that is exactly what the Smart Tissue Autonomous Robot (STAR) has promised to do. In a study at the Children’s National Medical Center in Washington, STAR could suture a pig’s bowel better, in terms of uniformity and quality of the sutures, than human surgeons (Greenemeier). Of course, this is simply just a start for the machine since STAR could soon begin to replace human surgeons in larger ways by being programmed how to make the primary incisions of surgery and cauterize, small but vital skills needed in the operating room (Zhang). At least for now though, doctors will need to do part of the procedure themselves. For instance, STAR relied on the surgeons in the suturing example “to make the initial incision, take out the bowel, and line up the pieces before it fired up its autonomous suturing algorithm” (Zhang). Nevertheless, if STAR does become fully autonomous, it may present a myriad of ethical problems to the medical community while also improving patient outcomes.

Smart Tissue Autonomous Robot in Action
IBM Watson could also greatly better patient outcomes by revolutionizing how doctors treat cancer along with other diseases. Using deep learning, Watson can take patients’ medical information, obtain important details, and make a treatment plan for the patient based on the latest evidence from resources online (Locklear). For example, Watson for Oncology has been trained by doctors at the Memorial Sloan Kettering Cancer Center to detect and diagnose cancer as well as to provide treatment options. More than eight out of ten times, Watson was accurate in diagnosing a patient with leukemia (Locklear). In addition, for lung and rectal cancer, Watson provided the same treatment recommendation as doctors did more than ninety percent of the time (Locklear). On top of all that, IBM Watson drastically reduced screening times by 78% for various different cancers, which is making everything quicker and more efficient (Locklear). Partnering with Boston’s Children Hospital, IBM Watson will also soon work to treat rare diseases in pediatric patients, focusing on steroid-resistant nephrotic syndrome (SRNS) first (Smith). Watson will learn nephrology by reading up on it online using natural language processing and supplement this knowledge with genetic information from patients with SRNS to make crucial connections that help find treatment options for the specific genetic mutations (Smith). The hope is that Watson will one day be able to use medical literature and the patient’s sequenced genome to diagnose rare diseases efficiently. One day, Watson may be also able to replace diagnosticians on a large scale as the technology advances more and more.
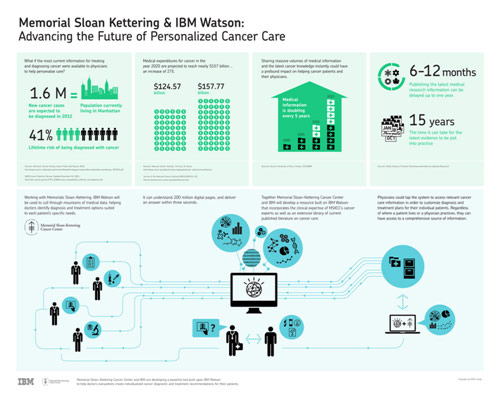
Infographic on Partnership Between Memorial Sloan Kettering & IBM Watson
Despite their forecasted benefits to patients, some of these types of automation have not been readily accepted by the medical community yet many are worried that humanity will lose something essential in health care if machines take over. The first main concern that has been widely voiced is in regard to the human touch. Human doctors have the role of healers, and a machine cannot give that same human touch when trying to obtain a patient history, for example, since a machine cannot empathize and communicate with a patient in the same way that a human can. Many people believe that doctors must always be there to reassure and satisfy their patients, having conversations with them to try to diagnose their ailment and to provide the answers for their various concerns (Zhang). Machines also may not ever be able to answer some of these concerns due to the black box problem. As mentioned before, systems learn how to distinguish between a variety of conditions by being fed medical images and diagnostic information (Mukherjee). By being given the diagnosis for many different presentations of diseases, these machines can form the pathways, or neural networks needed to get from the problem to the solution. Then with a slew of small adjustments, they become more specific and sensitive over time. However, the black box problem is that we cannot know what the machine is doing to make a certain diagnosis over another. Machine learning has made it so that it is impossible to decipher exactly how the machine is making connections and forming these neural networks (Mukherjee). Thus, when the patient asks why the machine cannot have the answer because it does not know why itself. With a completely automated system, we lose the benefit of knowing the answer to these types of questions. As Geoffrey Hinton, a computer scientist working at the University of Toronto, puts it, “the more powerful the deep-learning system becomes, the more opaque it can become” (Mukherjee). Finally, there is a major ethical aspect of autonomous machines in medicine. Machines cannot make moral decisions on their own, and they may actually get confused instead as shown in various different studies. For example, there was one study where a machine was programmed with the sole intention of not letting any other robot get into a danger zone. When there was only one other robot, everything went well; however, as soon as two other robots were present, this machine became confused and waited so long in forty percent of cases that both robots reached the danger zone (Meskó). Thus, ethics cannot be currently coded since attempting to do so forces programmers to consider infinite amounts of integral exceptions along with varying interpretations from culture to culture. To better understand why that is, consider a common ethical thought experiment, which asks “would you kill a baby to save 10 unnamed people?” Some people will say yes, arguing with a utilitarian mindset that we must do the greatest good for the greatest number. They will say that ten people are greater than one. Others will say no, arguing with a deontological mindset that the ends do not justify the brutal means. It is not ethically right to kill an innocent baby, even if it means saving ten unnamed people. Who is right, and who is wrong? Furthermore, what will we tell the machine is the right answer? All of these concerns may be answered, but in order for machines to become autonomous and more commonplace in medicine, the general perception is that they must be answered well.

Ethics Cloud
References
Alamy. A da Vinci Surgical Robot in USE to Treat a Prostate Cancer Patient. The Guardian, theguardian.com/technology/2014/oct/10/medical-robots-surgery-trust-future. Accessed 27 Sept. 2017.
Children’s National Medical Center. The Smart Tissue Autonomous Robot (STAR) Can Autonomously Perform 60 Percent of Bowel Anastomosis on Pig Intestines. PBS, pbs.org/newshour/rundown/new-robot-surgeon-sews-up-pig-intestines/. Accessed 27 Sept. 2017.
Greenemeier, Larry. “Robot surgeon sews up pig intestines.” 5 May 2016, pbs.org/newshour/rundown/new-robot-surgeon-sews-up-pig-intestines/. Accessed 28 Oct. 2017.
Infographic: Advancing the Future of Personalized Cancer Care CLOSE. Memorial Sloan Kettering Center, www.mskcc.org/blog/msk-trains-ibm-watson-help-doctors-make-better-treatment-choices. Accessed 27 Sept. 2017.
Locklear, Mallory. “IBM’s Watson Is Really Good at Creating Cancer Treatment Plans.” Engadget, 1 June 2017, engadget.com/2017/06/01/ibm-watson-cancer-treatment-plans/. Accessed 27 Sept. 2017.
Moral Character at SPSP 2014. SPSP, spsp.org/blog/moral-character. Accessed 27 Sept. 2017.
Mukherjee, Siddhartha. “A.I. Versus M.D.” The New Yorker, 3 Apr. 2017, newyorker.com/magazine/2017/04/03/ai-versus-md. Accessed 27 Sept. 2017.
“Robotic Surgery Institute.” University of Southern California Keck School of Medicine, cts.usc.edu/rsi-davincisystem.html. Accessed 27 Sept. 2017.
Smith, Steve. “5 Ways the IBM Watson Is Changing Health Care, from Diagnosing Disease to Treating It.” Medical Daily, 17 Dec. 2015, medicaldaily.com/5-ways-ibm-watson-changing-health-care-diagnosing-disease-treating-it-364394. Accessed 27 Sept. 2017.
Zhang, Sarah. “Why an Autonomous Robot Won’t Replace Your Surgeon Anytime Soon.” Wired, 4 May 2016, wired.com/2016/05/robot-surgeon/. Accessed 27 Sept. 2017.