On May 19th, I attended the Stanford Med School morning. It was an amazing experience that helped me learn more about some aspects of health care that I had not yet considered—from aspects of the medical school admissions process to the impact that a clinician-scientist can make. I learned quite a bit in the few hours that I spent in the Stanford lecture hall before we all went on the pavilion, going from stall to stall to see some of Stanford Medical School’s newest technology. For this post, I will focus primarily on the three speakers—professor of radiation oncology Dr. Iris Gibbs, professor of emergency medicine Dr. S.V. Mahadevan, and professor of plastic and reconstructive surgery Dr. Jill Helms. Each had a unique presentation that demonstrated some interesting part of medicine that is definitely worth sharing.

Stanford’s CHARIOT Program Stall: Using Virtual Reality to Curb Anxiety
Not only is Dr. Gibbs a professor of radiation oncology but also she is currently the associate dean of Stanford Medical School admissions and has received numerous accolades for her work. The primary focus of her presentation was to give all of us insight into what it takes to get into medical school and what the entire process entails. The process starts obviously with finishing high school and going to some college to do pre-medical studies. Interestingly enough, undergraduate students can study any subject matter and still go to medical school as long as they take rigorous pre-requisites like biology, physics, chemistry, and English that will help them study for the Medical College Admission Test, commonly known as the MCAT. Usually taken in the junior year, this standardized, multiple-choice test covers “Biological and Biochemical Foundations of Living Systems; Chemical and Physical Foundations of Biological Systems; Psychological, Social, and Biological Foundations of Behavior; and Critical Analysis and Reasoning Skills” (Princeton Review). After taking this exam, undergraduate students may apply for medical school in their senior year or take a gap year to pursue other interests.
Upon acceptance to medical school, they enter a world of rigorous studies. The initial years are in the classroom and are based on solidifying foundational scientific knowledge about the human body and its functions. At Stanford, this is coupled with “Scholarly Concentrations,” which is a program allowing medical students, with the guidance of a faculty member, to develop a project that is uniquely theirs and is based on their own interests. After these initial years, medical students will then work directly with patients and learn more about various specialties like surgery and internal medicine in 4-8 week clinical rotations. In the final year of medical school, students apply for residency positions and interview at hospitals around the US. The hospitals list their top choices, and individuals list their top choices. On Match Day, these students are “matched” to a hospital where they will spend the next 3-7 years. This specialized, hands-on training, known as a residency, marks the first time that these medical school graduates are practicing medicine by themselves; however, there is usually supervision. Afterward, doctors may elect to participate in fellowships or not, but it is important to note that medicine is a profession of lifelong learning. They must take a certain number of Continuing Medical Education (CME) courses and other licensing exams that happen periodically so that they stay sharp and current. In the words of Dr. Gibbs, becoming a doctor is more of a marathon than it is a sprint.
Dr. Gibbs then gave us greater insight into what Stanford looks at in their applicants. Before that though, she gave us a harrowing statistic. Out of the 49,990 people who applied to medical schools around the country, only 19,752 were enrolled, meaning only 2 out of 5 applicants in 2017 were enrolled in medical school. For Stanford Medical School enrollees in 2017, there were few interesting statistics. 85.1% had research or lab experience and 80.9% had experience with physician shadowing or clinical observation. They had an average of 54 courses on their application, their average GPA was 3.71, and their average MCAT score was 508.9 which is around the 75th percentile. These statistics help show what academic criteria Stanford is looking for in their medical students, yet that is only a part of their application. They also look for students with tenacity and determination, genuine concern and interest in people, strong communication skills, and an ability to think critically. Additionally, Dr. Gibbs emphasized the importance of students being unabashedly themselves and being like a stem cell, differentiating themselves from others in the application process. That is what sometimes makes a difference in Stanford’s holistic review, a “flexible, individualized way of assessing an applicant’s capabilities by which balanced consideration is given to experiences, attributes, and academic metrics” (Association of American Medical Colleges). For those they are interested in, Stanford conducts multiple mini interviews (MMI), which is a tool used to further assess an applicant’s personal attributes and skills. They want to find a great physician who will treat the patient with the disease, not just the disease. Thanks to Dr. Gibbs, I obtained an insight into Stanford’s and other medical school’s admission process.

Stanford Medical School Graduation
Dr. Mahadevan, in addition to being a professor of emergency medicine at Stanford Medical School, is also the founding director of the Stanford Emergency Medicine International and the lead editor of An Introduction to Clinical Emergency Medicine, a textbook that has won the AMWA Physician Category Textbook of the Year Award. He, along with Stanford ER physicians Dr. Jennifer Newberry and Dr. Monalisa Muchatuta, examined an episode from the TV show “E.R.” This episode specifically concerned a patient named Steve Curtis, who is a 35-year-old detainee. He had diffuse, achy abdominal pain for 6 hours that was resolved once in the hospital. He vomited once and had no diarrhea. He has a blood pressure of 124/80 and a temperature of 99.4°F. The senior doctor examining him in the show seemed to dismiss his concerns and gave him a diagnosis of stomach flu. However, this doctor showed obvious signs of bias against this detainee.
At this moment, Dr. Mahadevan paused the video and asked Dr. Muchatuta and Dr. Newberry about their thoughts. Dr. Muchatuta commented on the importance of developing a differential diagnosis, which is a list of possible causes for the symptoms the patient has. ER doctors tend to first think of the worst possible diagnosis since they do not want to miss important signs that could prove life-threatening. For this patient in mind, some of the differential diagnoses that Dr. Muchata was thinking of included appendicitis (inflammation of the appendix), kidney stones (mineral/salt deposits formed in the kidney), and diverticulitis (inflammation of some pouches in the digestive tract). Dr. Muchata emphasized the importance of “ruling out appy,” or making sure the condition was not appendicitis since this condition often requires an emergency surgery called an appendectomy. Dr. Newberry then came in and talked more about appendicitis, explaining how the infection can be caused by little pieces of food or feces stuck in the appendix. In regards to examination findings, Dr. Newberry talked about abdominal guarding and rebound tenderness that occurs when the ER doctor presses their hand on the patient’s abdomen. Abdominal guarding refers to the tensing of the abdominal muscles to protect inflamed organs from pressure. Clinically, it is characterized by the patient clenching their abdomen or swatting the ER doctor’s hand when they try to press the patient’s abdomen. Rebound tenderness, or Blumberg’s sign, refers to intense pain that follows the quick release of the ER doctor’s pressure on the lower-right abdomen. Other tests Dr. Newberry said she might consider included blood tests to rule out or add to her differential diagnosis list and an abdominal ultrasound that would strongly point towards appendicitis if there was an enlarged non-compressible appendix greater than seven millimeters. The two doctors then both criticized the TV doctor’s bias and dismissal of the patient’s symptoms before continuing the video.
In the remainder of the clip, we saw the junior doctor worry about the patient’s status while the senior doctor just wanted to send him back to prison. However, the senior doctor agrees to check the patient once again and sees that the patient has lost consciousness, has a temperature of 100.4°F, has rapidly falling blood pressure, and has increased white blood cell count to 12,000 (left-shift). The video was paused again so that Dr. Muchatuta and Dr. Newberry could explain that what probably happened was that the patient’s appendix ruptured, so the infected material went to his blood, making it harder for blood to flow to the brain and causing sepsis. Dr. Mahadevan commented that there were a few things we could learn from this case. First, doctors must treat all patients the same, regardless of who they are or what their background is, in order to provide high-quality care. Second, developing a differential diagnosis with the help of the patient and the team is really important to prevent serious complications from occurring. The doctor’s diagnosis of stomach flu was a potential diagnosis, but stomach flu should not have been on the top of this doctor’s list since other possible conditions were significantly more serious. Dr. Mahadevan’s talk gave me a greater appreciation for the complexities of medicine in the emergency room setting and while also teaching me a lot about appendicitis.
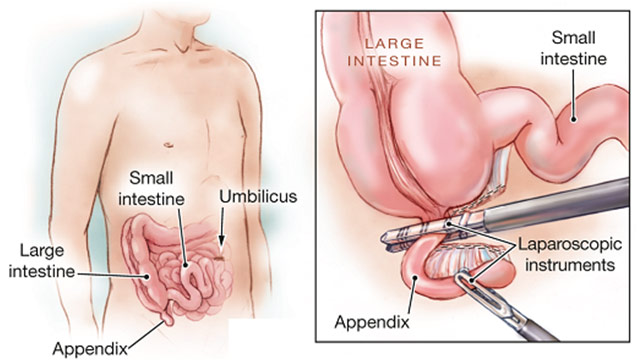
Laparoscopic Appendectomy for Appendicitis
Dr. Jill Helms not only is a professor of plastic and reconstructive surgery at Stanford Medical School but also is the recipient of numerous accolades like the Distinguished Scientist Isaac Schour Memorial Award, which is the highest honor given by the International Association of Dental Research. She spoke on what it means to be a clinician-scientist while also shedding some light on her work in stem cell research. First, she talked about how you can really blaze your own path to become a clinician-scientist, obtaining any combination of clinical degrees (MD, DDS, DVM) and research degrees (Ph.D., MS, MPH). She then went on to discuss how clinician-scientists are creative, risk-takers, and, most importantly, are willing to fail. After all, it is called research not just search. These traits allow clinician-scientists to tackle some of the biggest medical problems in the world by doing research, making discoveries, and constantly innovating.
Clinician scientists must also be willing to spend most of their time simply exploring in order to make amazing findings to various medical problems. Take bone marrow transplants for leukemia for example. In an ideal world, everyone with leukemia would have a healthy twin who could donate their bone marrow. A similar genetic profile would reduce the risk of transplant rejection as the bone marrow would be more compatible with the recipient’s immune system. However, we live in a realistic world where this is simply not the case. Clinician scientist Dr. Irving Weissman tried to solve this problem by isolating the first hematopoietic stem cells, which have the unique capacity to make exact copies of themselves and to give rise to all other blood cells. They help the bone marrow transplants be more successful by improving engraftment rates, which in turn increase patient survival rates. Thanks to the work of other clinician-scientists, we also now know that hematopoietic stem cells can be recovered from the umbilical cord, which is regarded as medical waste in most hospitals. The stem cells from this “waste” can then be frozen so they can be used in the future for absolutely anybody who needs it. Through this example, Dr. Helms showed how the work of clinician-scientists changes lives.
Dr. Helms also spoke on her own research as a clinician-scientist in relation to a problem that arises after the surgical repair of a cleft lip and palate, a craniofacial abnormality characterized by a separation of the upper lip and roof of the mouth. Surgery is done to close this separation or gap, but it tends to leave a scar that impedes the growth of the “upper jaw, cheekbones and eye sockets” (midfacial hypoplasia) according to St. Louis Children’s Hospital. Dr. Helms started to consider if there was a better way: if, some way or the other, she could regenerate the bone. She submitted a grant to the National Institute of Health (NIH) and California Institute for Regenerative Medicine (CIRM), and after being denied a few times, she got funding from CIRM for this project that would eventually cost $12 million. The basis behind her project was to activate the osteoprogenitor cells, stem cells that already exist in a patient with a cleft lip and palate and can differentiate to become bone, with a stem cell-activating protein called “Wnt.” After testing this hypothesis on animal models with bone injuries, Dr. Helms found that the Wnt protein was indeed successful in forming the bone sooner when compared to a control. Since Stanford University owns the license to any technology Stanford researchers develop in their lab, they licensed the technology to a group of venture capitalists, who founded a company called Ankasa Regenerative Therapeutics, Inc. in San Francisco. Similar to the example with Dr. Weismann, Dr. Helms proves how the work of clinician-scientists can make enormous differences in people’s’ lives.
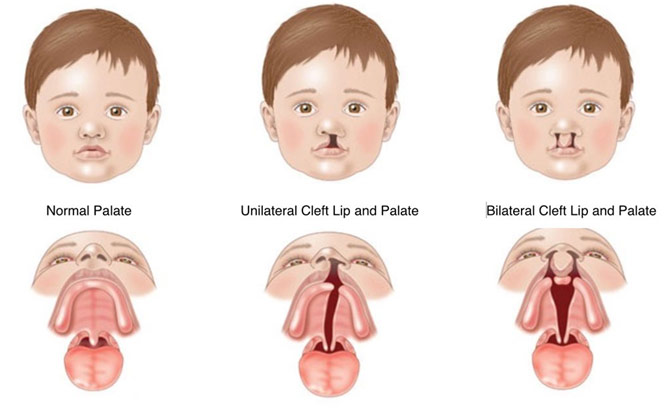
Normal Palate vs. Cleft Lip and Palate
Stanford Med School Morning was an amazing experience to hear and learn from some doctors who are at the absolute pinnacle of their fields. It was an honor to hear from them, and it inspired me, and everyone else I am sure, to work harder to make it to this point where these amazing doctors have reached. Thank you to Stanford Medical School and these kind doctors for organizing this event to inspire the next generation of health care workers!
References
Bennington-Claro, Joseph. “Symptoms of Appendicitis: Nausea, Fever, Abdominal Pain, and More.” Edited by Robert Jasmer. Everyday Health, 30 May 2018, www.everydayhealth.com/g00/appendicitis/guide/symptoms/?i10c.encReferrer=&i10c.ua=1&i10c.dv=14. Accessed 9 June 2018.
Cleft Lip and Cleft Palate. Craniofacial Team of Texas, craniofacialteamtexas.com/cleft-lip-and-cleft-palate/. Accessed 9 June 2018.
Discover What Matters. Med School Morning Registration, events.attend.com/f/1383784237#/reg/0/. Accessed 9 June 2018.
Fisch, Steve. Stanford Medicine – Stanford ‘18. Instagram, www.instagram.com/p/Bi2Wk6jF2HU/?taken-by=stanford.med. Accessed 9 June 2018.
“Holistic Admissions.” Association of American Medical Colleges, www.aamc.org/initiatives/holisticreview/about/. Accessed 9 June 2018.
Howard, Christopher. Stanford Medicine – Health Matters 2018. Instagram, www.instagram.com/p/Bja6nLAlWjh/?taken-by=stanford.med. Accessed 9 June 2018.
Laparoscopic Appendectomy Surgery. Health Press, healthpress.me/appendectomy-recovery-time-healing-to-go-back-to-work/. Accessed 9 June 2018.
“MCAT Sections: What’s on the MCAT?” The Princeton Review, www.princetonreview.com/medical/mcat-sections. Accessed 9 June 2018.
“Midfacial Hypoplasia.” St. Louis Children’s Hospital, www.stlouischildrens.org/our-services/plastic-surgery/midfacial-hypoplasia. Accessed 9 June 2018.